Many people out there have jobs that require long hours on hard floors, and their feet suffer for it. In the next two posts, I want to discuss some tips on how shield the feet from the strain that those long hours can inflict on them, and how appropriate shoes and inserts can help makeContinue reading “Shoe Advice For Those That Work Long Hours On Their Feet”
Tag Archives: foot pain
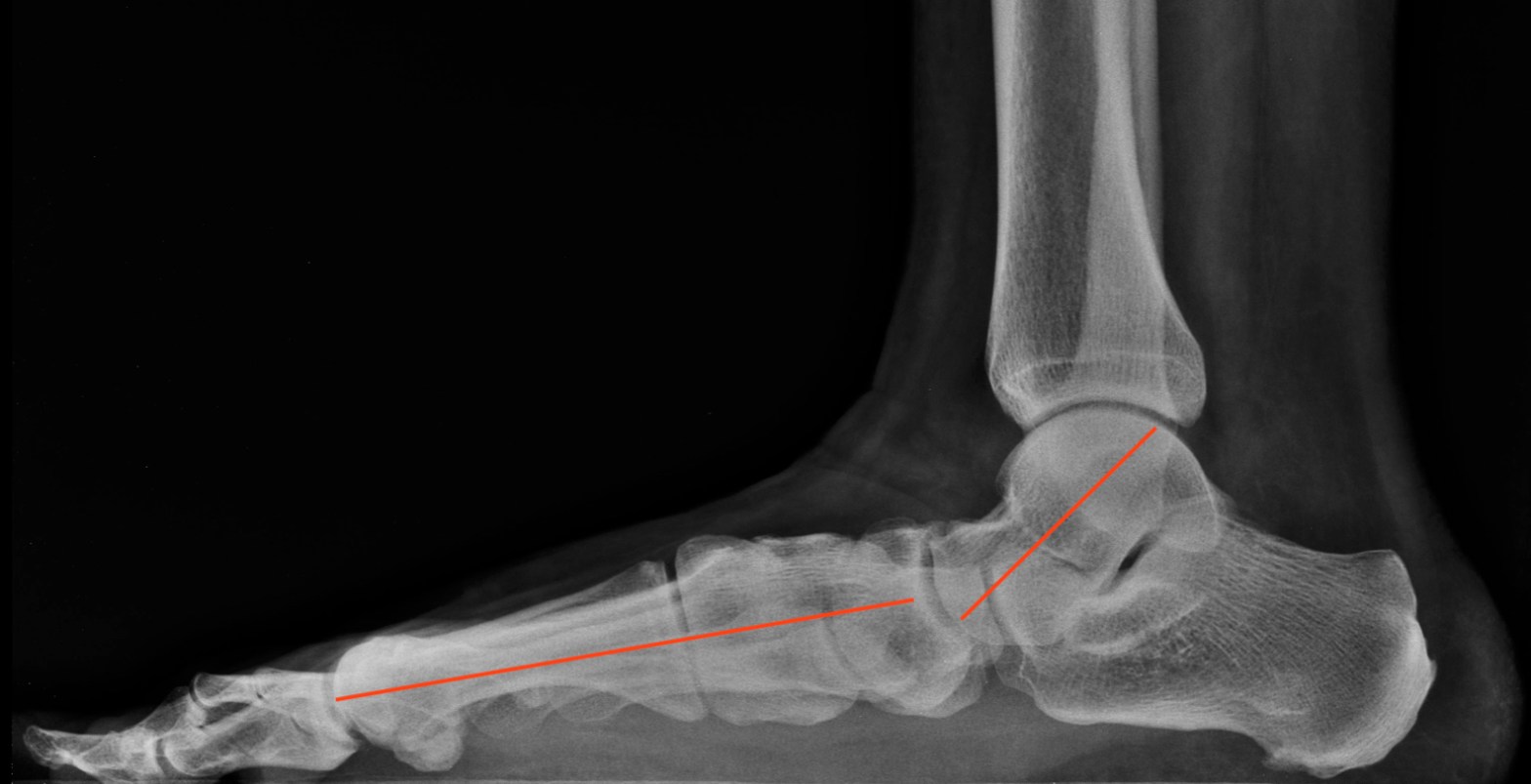
Flat Feet Explained Final Part: Surgical Treatment
This week, I will conclude my discussion on the treatment of flat fee by discussing surgical correction. Surgery is usually reserved for people who have failed orthotic therapy, or those who have rigidly flat feet that generally will not benefit from orthotic inserts. Each surgeon has their own criteria regarding how early they consider surgicallyContinue reading “Flat Feet Explained Final Part: Surgical Treatment”
Flat Feet Explained: Part 2 Non-Surgical Treatment
This week, I am continuing my discussion on the treatment of flat feet in teens and adults. We are now ready to discuss treatment options. In basic terms, there are two options for treatment, as there are two basic types of flat feet. The options are supportive shoes and prescription orthotics inserts, and surgical reconstruction.Continue reading “Flat Feet Explained: Part 2 Non-Surgical Treatment”
Flat Feet Explained: Part One
Over the next couple of weeks I would like to discuss the nature of painful flat feet in the older child/teen and adult, and share some of my thoughts on treatment of this foot deformity. Since this is a fairly involved topic, splitting the discussion up will help keep the post from getting too ‘wordy‘.Continue reading “Flat Feet Explained: Part One”
Pain Under the Big Toe Joint: Sesamoiditis
Pain under the big toe joint can be a significant nuisance, and can make walking, squatting, and jumping painful. This pain is typically due to a common condition called sesamoiditis. Sesamoiditis is inflammation of one of two small, egg-shaped bones found under the big toe joint., known as the sesamoid bones. Every human has them,Continue reading “Pain Under the Big Toe Joint: Sesamoiditis”
Don’t Ignore Achilles Tendonitis and Pain In the Back of Your Heel
The Achilles tendon- a potential weak point of many an athlete and warrior. It can hobble the mighty, and make life difficult for anyone unfortunate enough to injure it. So-named for the weakest part of the great Greek warrior Achilles, who was invulnerable through being dipped into the river Styx at birth, except for theContinue reading “Don’t Ignore Achilles Tendonitis and Pain In the Back of Your Heel”
When Should I Have My Bunion Operated On?
Bunions, for those who suffer with them, can be very painful, or may never cause a moment of discomfort. This foot deformity, in which the base of the big toe is prominent on the inner side of the foot and the big toe itself is angled toward the second toe, has been covered by meContinue reading “When Should I Have My Bunion Operated On?”
Plantar Fascia Tears: A Dreaded Sports Injury
Plantar fascia tears are infrequent but relatively common athletic injuries involving a ligament on the bottom of the foot in the arch, and can cause significant pain and disability in sports and daily activity. It usually is an injury that sidelines most lower level athletes and makes daily walking difficult for non-athletes. The plantar fasciaContinue reading “Plantar Fascia Tears: A Dreaded Sports Injury”
Is a neuroma really a pinched nerve?
A neuroma is a common foot malady that does indeed involve a nerve in the foot, and is often described by health care professionals, general medical doctors or orthopedists, and even podiatric specialists as being a pinched nerve. This is often done to simplify the medical language for a patient, but I think when myContinue reading “Is a neuroma really a pinched nerve?”
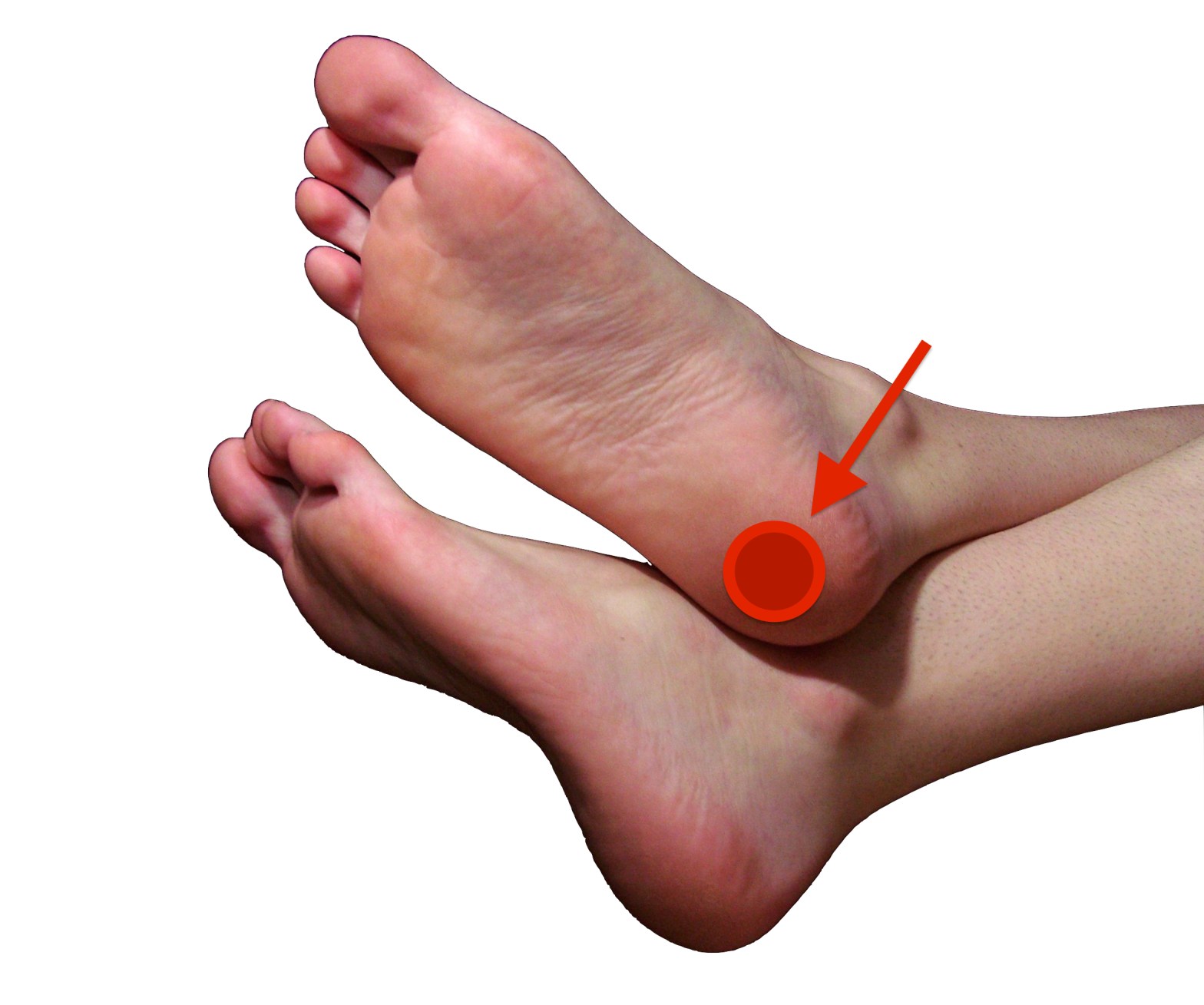
Did you know you can get bursitis in your heel?
While most cases of pain on the bottom of the heel are caused by plantar fasciitis, some are not. A common alternate cause of heel pain is a condition called bursitis, and it can lead to severe pain directly on the bottom of the heel. Bursitis is inflammation of a bursal sac, which is aContinue reading “Did you know you can get bursitis in your heel?”