Foot pain can have many different causes, and sometimes the actual cause is not immediately clear if the pain feels like it is spread over a wide area. Fortunately, the nature of the pain itself can sometimes provide a clue as to the actual origin. It is not uncommon in cases where pain is feltContinue reading “The Nature of Your Foot Pain Can Clue You As To the Cause”
Monthly Archives: June 2017
Pain on the outside of your foot? It could be due to peroneal tendonitis.
A common foot injury often misdiagnosed as a complex ankle sprain is called peroneal tendonitis. The peroneal tendons are two in number, and run together under the outside of the ankle joint, where they stay together for a couple inches until they reach the middle part of the side of the foot. It is hereContinue reading “Pain on the outside of your foot? It could be due to peroneal tendonitis.”
Is a neuroma really a pinched nerve?
A neuroma is a common foot malady that does indeed involve a nerve in the foot, and is often described by health care professionals, general medical doctors or orthopedists, and even podiatric specialists as being a pinched nerve. This is often done to simplify the medical language for a patient, but I think when myContinue reading “Is a neuroma really a pinched nerve?”
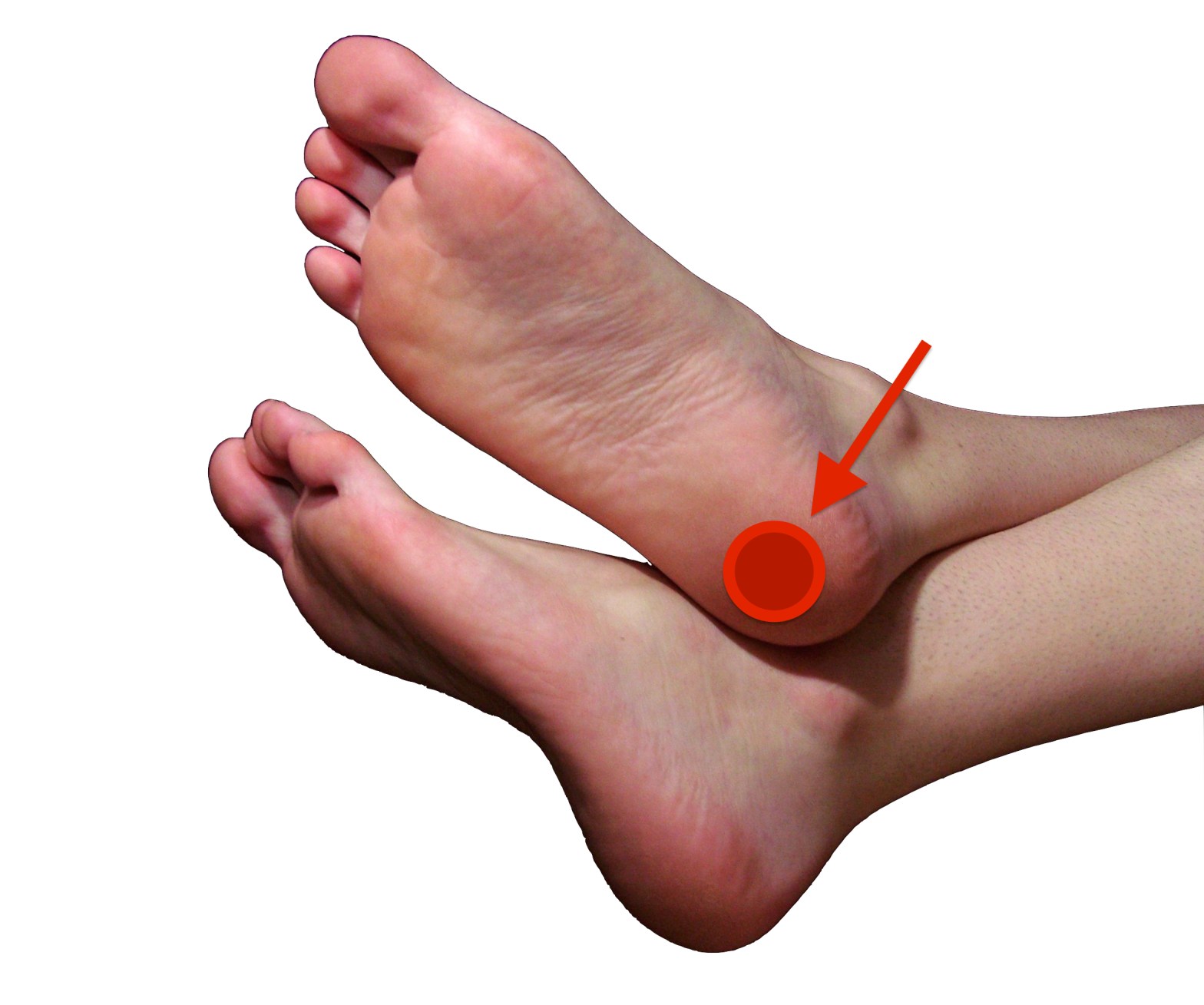
Did you know you can get bursitis in your heel?
While most cases of pain on the bottom of the heel are caused by plantar fasciitis, some are not. A common alternate cause of heel pain is a condition called bursitis, and it can lead to severe pain directly on the bottom of the heel. Bursitis is inflammation of a bursal sac, which is aContinue reading “Did you know you can get bursitis in your heel?”