Many people experience discomfort and hardness to the outside of the little toenail, and assume it is because of an ingrown toenail or a hang nail. They trim the nail back at this side, and maybe even have their doctor remove the side of the nail, but the problem seems to keep coming back. WhyContinue reading “If You Think You Have an Ingrown Toenail On the Outside of Your Little Toe…..You May Be Wrong”
Monthly Archives: March 2017
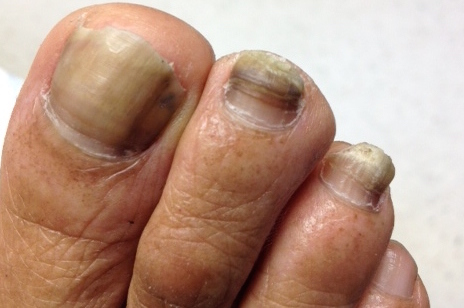
What Can Be Done About A Thick and Painful Toenail?
Many people are surprised to find out that toenails are relatively fragile appendages of the body. Toenails can take a mild amount of abuse from tight shoe pressure, years of toe stubbing or objects dropping on them, damage from jogging and exercise, or changes due to chronic fungus infections. Over time though, the nail rootContinue reading “What Can Be Done About A Thick and Painful Toenail?”
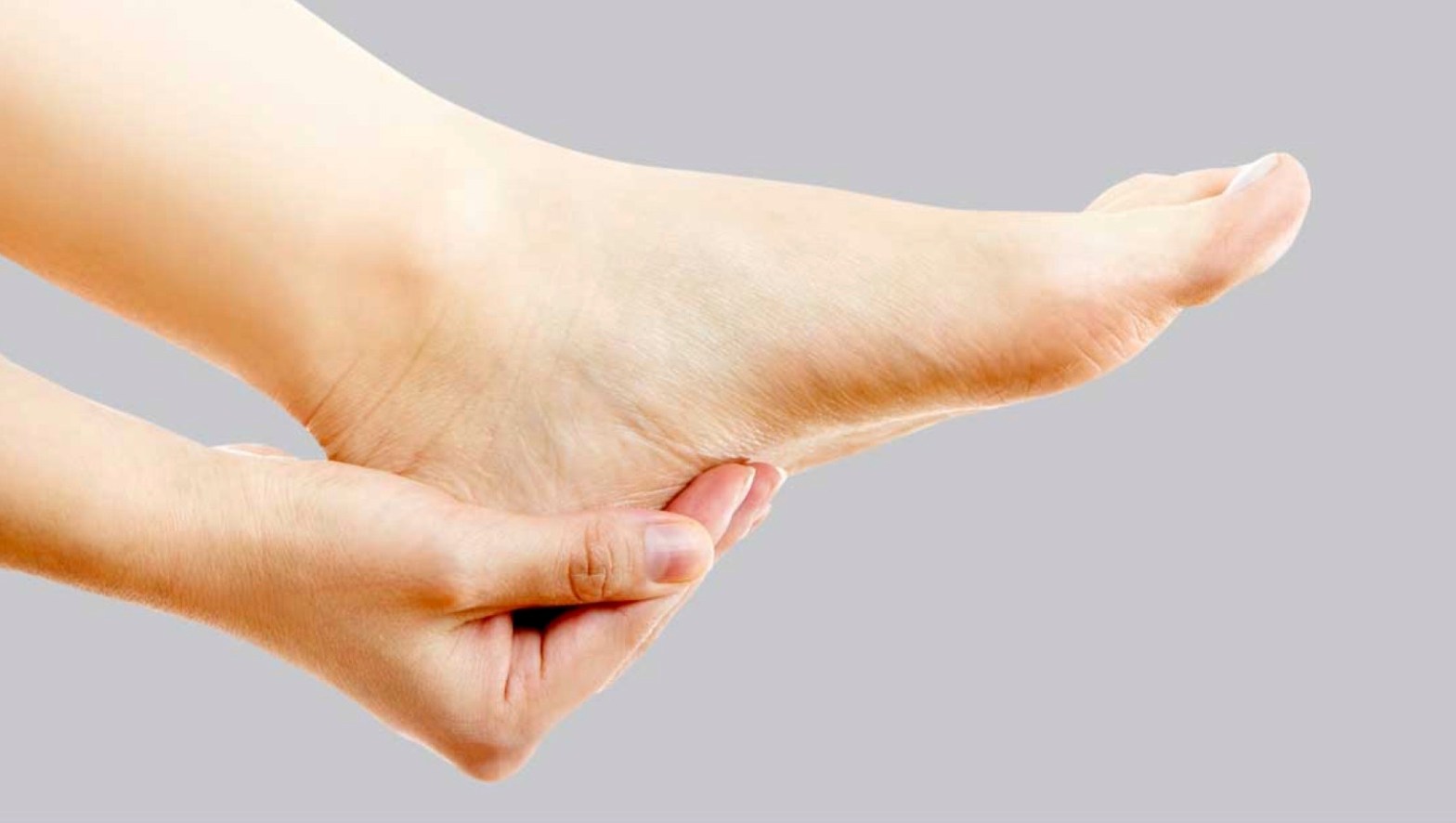
I Felt A Sharp Pain With A Snap In My Arch When I Stepped Down and Now I Can’t Walk
Some of the most frequent foot injuries I see involve the heel and arch. A number of different injures can cause pain in this part of the foot, including muscle and tendon strains. However, one structure by far sees the most number of injuries in this region: the plantar fascia. The plantar fascia is aContinue reading “I Felt A Sharp Pain With A Snap In My Arch When I Stepped Down and Now I Can’t Walk”
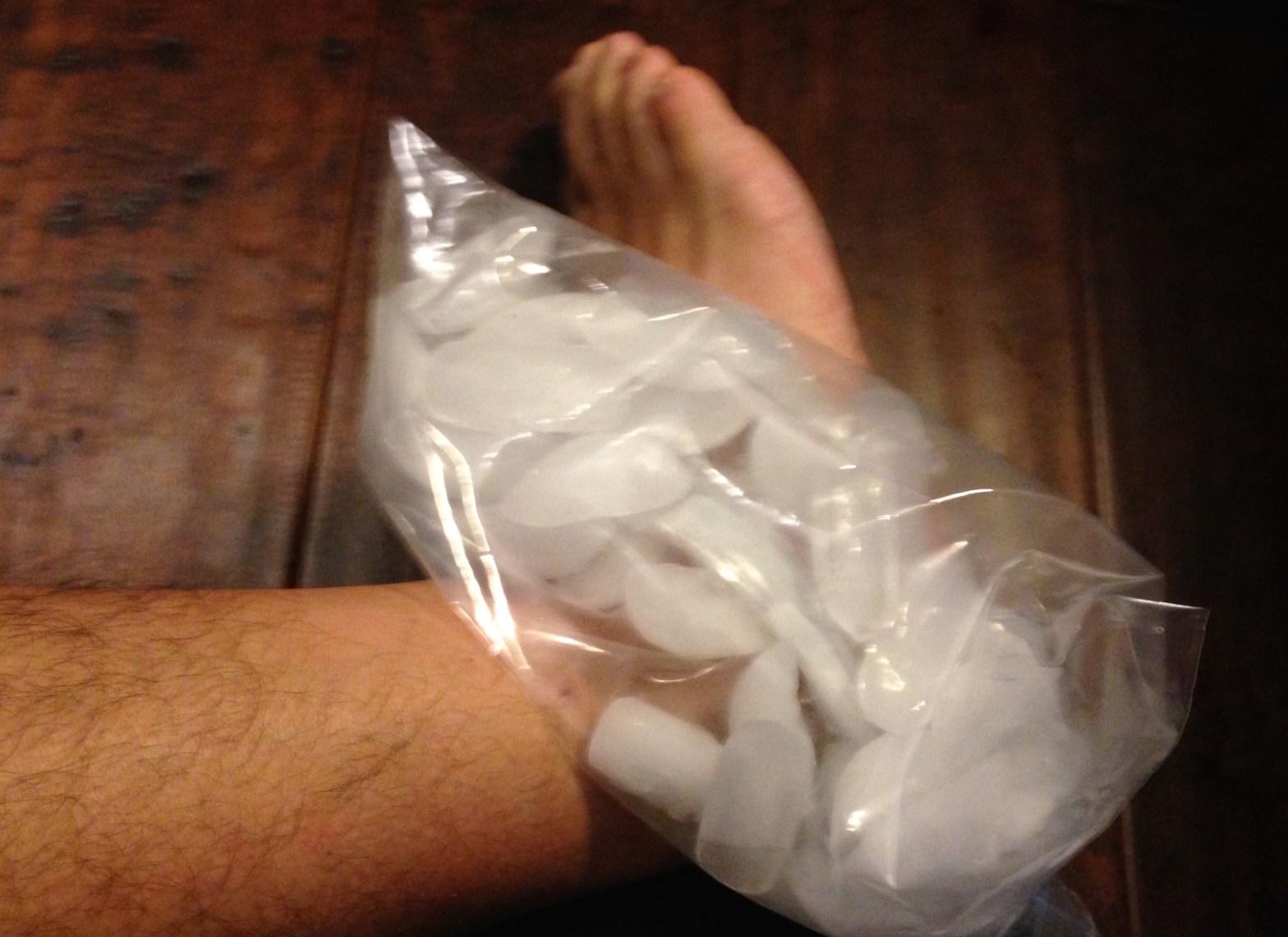
Do I Need To See A Doctor For My Anke Sprain?
Ankle sprains are one of the most common injuries that occur in the body. Athletes playing sports make up part of the millions of people each year who sprain their ankle, as well as people simply walking on uneven ground, stepping into a hole, slipping on ice, or awkwardly stepping off of a curb. AnkleContinue reading “Do I Need To See A Doctor For My Anke Sprain?”