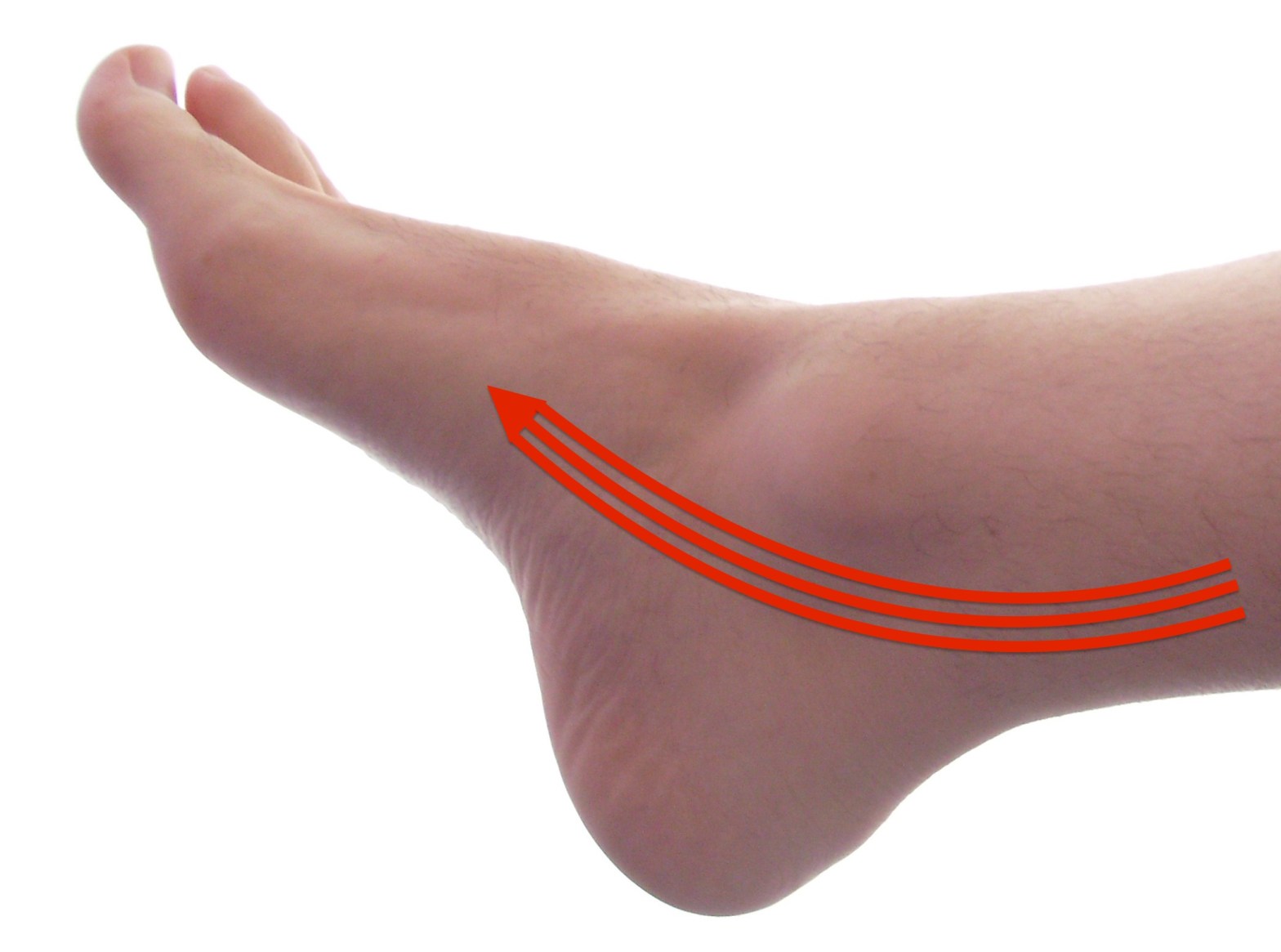
Posterior tibial tendonitis and tendon dysfunction are related inflammatory and degenerative conditions that involve an important tendon that runs under the inner side of the ankle and attaches further down into the inner side of the foot. This tendon and its attached muscle curl the foot inward and resists the foot’s tendency to flatten out, and stabilizes the foot while walking and standing.
People with flat feet often damage this tendon gradually as it is stretched over the side of the foot during the flattening motion. Those with normal arches can also injure this tendon when walking on uneven surfaces or during sprains. The initial stage of this disease is simple inflammation and microscopic tendon damage, or tendonitis. In this stage as a whole the tendon is still intact and relatively healthy. If untreated, this disease process will continue to worsen, until the more serious posterior tibial tendon dysfunction develops. The tendon becomes weak and unable to effectively support the foot, and as a result the foot flattens out further. Eventually, the foot will become so unstable that it is functionally limited, and aggressive treatment must be performed to restore the ability to walk properly.
Early symptoms can include pain, swelling, warmth, or tightness to the foot on it’s inner side. This pain may be felt in an area under the ankle all the way to the middle part of the foot on that side, and there can even be pain in the inner side of the lower leg as well if the muscle is involved, although this is uncommon. The pain is worse when walking barefoot, and may feel better in a supportive athletic shoe. It can start suddenly, can follow an injury, or can develop gradually. If untreated, the foot will become weak on that side, and will visibly flatten further.
Treatment is involves halting the inflammatory process and providing immediate support to the weaker tendon to help it heal. Rest, ice, anti-inflammatory medications, and the use of a gauntlet-style ankle brace are the initial treatments of choice. Physical therapy or immobilization in a pneumatic walking boot may also be necessary. Cases that persist beyond these treatments, or cases that enter the later stages of posterior tibial tendon dysfunction may require surgical intervention. During surgery for this condition, the tendon is repaired and augmented with various modern techniques that can include strengthening grafts, radiofrequency wave treatment to stimulate blood flow, or platelet gel application to stimulate internal healing. Special braces that combine ankle and foot support may be needed to prevent further foot collapse, and the severe cases that may involve joint damage from the deformity caused by the advancing foot flattening may require fusion of foot bones to stop the arch collapse permanently.