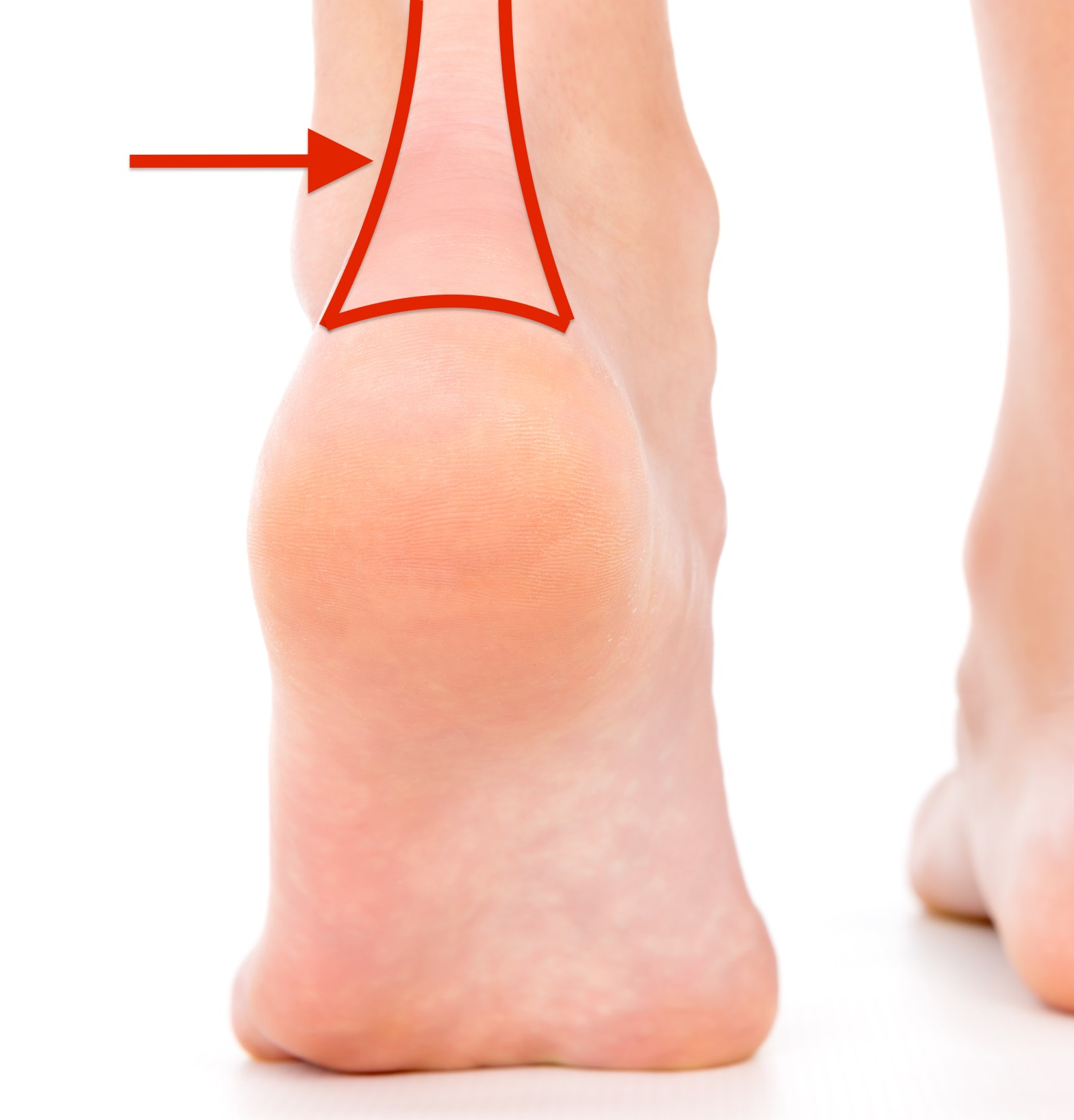
Achilles tendonitis occurs when there is damage and inflammation to the Achilles tendon, a thick strap-like tendon found behind the ankle and heel. The Achilles tendon is a combination of the tendons of muscles in the calf called the gastrocnemius and the soleus. These muscles act to flex the foot downward, which resists the force of the ground trying to push the foot upward when one is walking. The tendon is generally strong and thick, but it can become weakened through injury or chronic stress, leading to inflammation and tendon degeneration.
The Achilles tendon can be injured in one of several different ways. One way occurs during sports or heavy activity. This is usually seen when the foot is suddenly flexed upward and the tendon is stretched behind the heel, such as when landing hard on the ball of the foot from a jump or coming off of a step awkwardly. The tendon can also be damaged if someone else directly lands on the heel. If the force is great enough, the tendon can actually tear. Another way the Achilles tendon can be injured is during an accident, such as a minor car wreck in which the foot is braced on a brake during impact, or if the Achilles tendon is directly struck by a heavy falling object or swinging object like a closing door. The most frequent way people develop Achilles tendonitis is from chronic strain. This can occur during the activities of daily life if the tendon is tight, or if one has feet that flatten out too much. Tightness of the tendon can lead to strain as the body weight forces the tight fibers to stretch beyond what they are easily capable of. Excessive flattening of the feet, or overpronation, can strain the fibers of the Achilles tendon because the heel bone rotates outward during this process, which in turn causes some stretching of the Achilles tendon where it attaches to the heel bone. Over time, these two factors will cause gradual tendon strain that leads to inflammation, pain, and tendon damage.
The tendon can also be irritated by spurs or bony enlargements on the back of the heel bone, and the tendon tissue itself can develop calcified areas..
The symptoms of Achilles tendonitis may include a sharp pain to the back of the heel or just above it, and a dull achy pain when not active. The pain may worsen when the foot is stretched upwards, but not always. Achilles tendon pain can feel worse after a period of inactivity when the tendon stiffens further. Furthermore, the tendon can also hurt simply from pressure by the back of a shoe. Noticeable skin swelling around the tendon is possible, but not common, although the tendon can feel enlarged and lumpy to the touch where it is inflamed and damaged.
Treatment of Achilles tendonitis involves actively reducing the inflammatory process stabilizing the tendon so it has a chance to heal, and keeping the tendon limber to prevent future injury. Inflammation can be reduced by anti-inflammatory medications, icing, and rest. Injections are often requested by patients but not recommended in this area because the medication can weaken the tendon and cause a rupture. The tendon usually is best stabilized by employing a high quality ankle brace to resist excessive ankle motion under the load of body weight. This is typically worn during all activity, including at home. However, in spite of this stabilization, the Achilles tendon needs better mobilization to increase its flexibility and reduce the potential for strain. Stretching exercises and physical therapy are the mainstays of this treatment, and night splints are also sometimes used. Finally, prescription orthotic shoe inserts are often used to control overpronation if it is present to reduce heel bone rotation and Achilles strain in the long term.
Severe cases of tendonitis may need surgery to repair the tendon or stimulate it to heal. This is especially the case if there are partial tears present in the tendon, or if bone spurs are present that continuously irritate the tendon. If the tendon ruptures, it needs immediate surgical repair as delayed treatment can lead to great difficulty in repairing it due to tendon stump retraction and scar tissue formation.